Your hair transplant surgeon spent hours placing thousands of grafts with surgical precision. But here's what most patients don't realize: how you sleep over the next 7–10 nights matters almost as much as what happened in the operating room. Sleep on your back, elevated at a 45-degree angle, for at least 7–10 nights. That's the essential rule — and this guide will show you exactly how to follow it, night by night, from your clinic bed in Istanbul to your own bed at home.
*This guide provides general aftercare information based on widely accepted clinical practices. It is not a substitute for the specific post-operative instructions provided by your surgeon. Always follow your surgeon's personalized guidance, as individual cases may vary.*
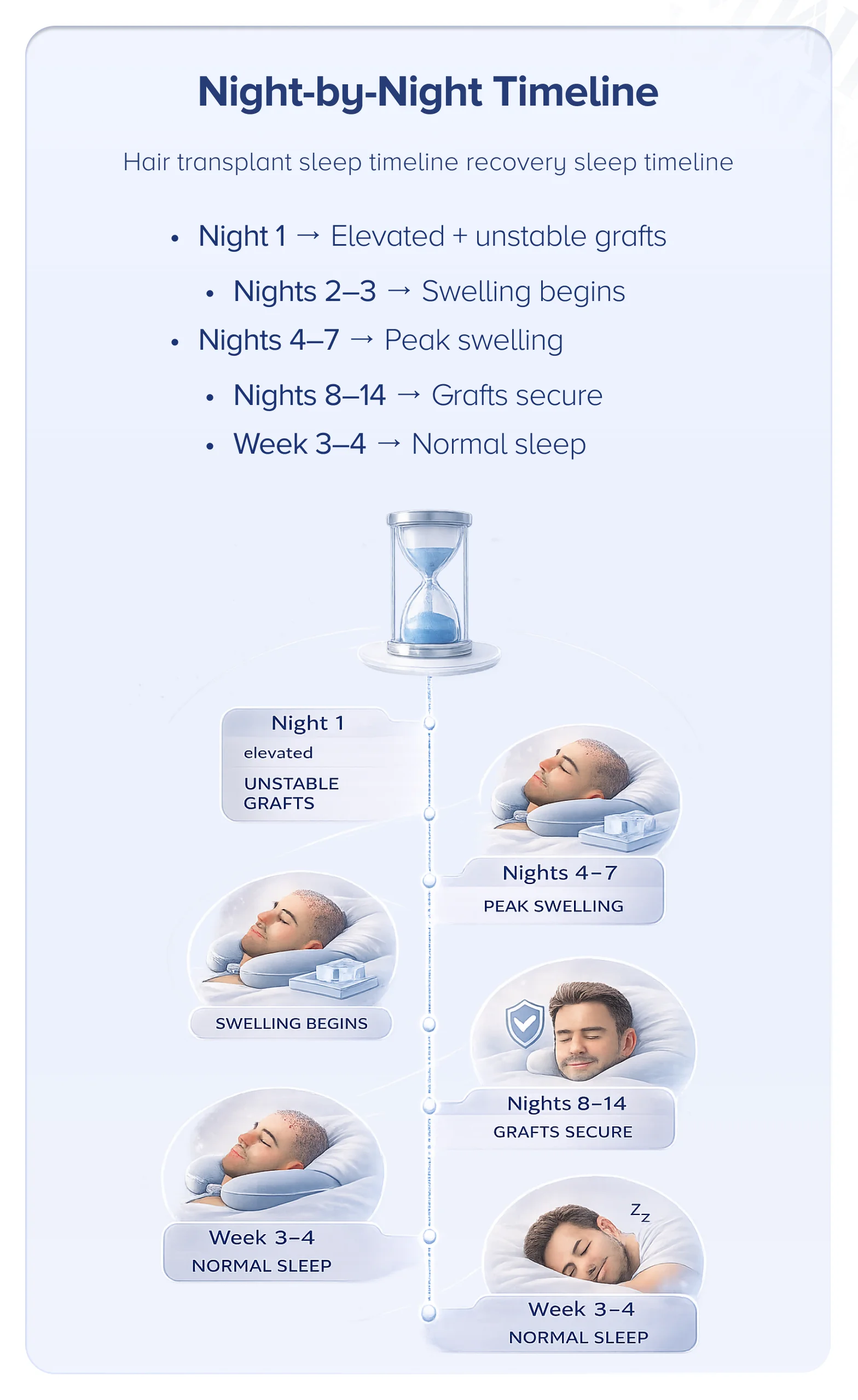
Sleeping after a hair transplant is one of the most common concerns patients raise — and one of the most important aspects of hair transplant recovery sleep. Below, you'll find a complete night-by-night timeline, the best sleeping positions explained with medical reasoning, practical setup tips, advice for the flight home, and answers to every common question. For the full picture of post-operative care beyond sleep, see our complete hair transplant aftercare guide.

Why Sleeping Position Matters So Much After a Hair Transplant
You know the core rule — 45 degrees, 7–10 nights. But understanding why makes all the difference in actually following through, especially on Night 4 when your patience is wearing thin. Three biological factors make your sleep position critical during the first two weeks.
How New Grafts Anchor Into the Scalp
Think of each newly transplanted follicle like a seedling placed into fresh soil. It needs time to take root before it can handle any disturbance. Transplanted hair follicles (grafts) sit in tiny incisions in your scalp, and they are not locked in place right away.
Over the first few days, your body begins a process called neovascularization — the formation of new blood vessels that supply the transplanted follicles with blood and nutrients. This process typically starts around Day 3–4. However, grafts are generally not considered secure until roughly Day 10–14.
During this window, direct friction, pressure, or rubbing against a pillow can dislodge grafts before they've established their new blood supply. Every sleeping instruction in this guide exists to protect those fragile follicles while they anchor.
The Role of Swelling and Blood Flow
Lying flat increases blood flow to your head, which worsens post-operative swelling. This swelling typically peaks between Days 3–5 and often shows up as puffiness in the forehead and around the eyes.
Elevating your head works the same way elevating a sprained ankle does — gravity helps drain excess fluid away from the area. Keeping your head above your heart reduces fluid accumulation and helps you heal faster. Excessive swelling isn't only a cosmetic concern — it can slow the healing process and increase discomfort significantly.
Donor Area Sensitivity
The donor area — the back and sides of your head where follicles are harvested — will be tender after your procedure. This is especially true after Follicular Unit Extraction (FUE), which leaves hundreds of tiny micro-wounds across the donor zone.
Even if your transplant area is on top of your head, the donor area at the back creates a real problem. Lying flat on a regular pillow puts direct pressure on those healing wounds. Donor area tenderness is another key reason why elevated back sleeping is the recommended position from Night 1.
Here's a quick summary of why position matters:
● Graft protection: Newly placed follicles need 10–14 days to anchor securely through new blood vessel formation.
● Swelling control: Elevation uses gravity to reduce fluid buildup, especially during the Day 3–5 peak.
● Donor area comfort: Sleeping flat puts direct pressure on healing micro-wounds at the back of your head.
Quick Quote in 5 Minutes
Talk to an experienced patient coordinator for your hair transplant in Turkey.The Best Sleep Position After a Hair Transplant
Now that you understand why your sleeping position after hair transplant is so critical, here's exactly how to position yourself — and when each position becomes safe.
Elevated Back Sleeping: The Gold Standard
Sleeping on your back at a 30–45 degree angle is the single best position for the first 7–10 nights. This is consistent with guidelines from the International Society of Hair Restoration Surgery (ISHRS) and recommended by virtually every reputable hair transplant surgeon. Some surgeons advise 30 degrees, others 45 — follow your surgeon's specific guidance.
Here's how to set it up:
● Use 2–3 firm pillows stacked to create a gradual incline, or use a wedge pillow for consistent elevation.
● Place a small pillow under your knees to relieve lower back pressure — this makes back sleeping far more comfortable.
● Add a U-shaped travel neck pillow around your neck to keep your head centered and prevent it from rolling to either side.
● A recliner chair is another excellent option, especially if you're not used to sleeping on your back.
Your head should remain higher than your heart at all times during sleep. This position protects the transplant area from pillow contact and keeps swelling under control.
If you have a medical condition that makes back sleeping difficult — such as chronic back pain, severe acid reflux, or a respiratory condition — discuss this with your surgeon before your procedure. They can provide alternative positioning guidance tailored to your situation.
Can You Sleep on Your Side After a Hair Transplant?
If you're wondering when you can sleep on your side after a hair transplant, the short answer is: not for the first 7–10 days. This is especially important if grafts were placed on the top or front of your scalp.
Even if the grafts aren't directly touching the pillow, side sleeping causes your head to tilt. This can create unexpected contact between the transplant area and the pillow surface, and it doesn't help with swelling control either.
If your transplant was limited to the crown area, gentle side sleeping may be cautiously possible a few days earlier — but only with your surgeon's explicit approval. After Day 10–14, most surgeons allow gentle side sleeping as grafts become significantly more secure.
Can You Sleep on Your Stomach After a Hair Transplant?
Stomach sleeping is the highest-risk position after a hair transplant. It places direct, sustained pressure on the transplant area and causes maximum swelling by keeping your head level with — or below — your heart.
Avoid sleeping on your stomach for at least 4 weeks — ideally longer. This is the last sleep position to reintroduce. Your surgeon may advise waiting even longer depending on your healing progress. If you're naturally a stomach sleeper, the pillow barrier method described in the tips section below will be especially important for you.
FUE vs. DHI: Does the Technique Change How You Sleep?
The core sleeping advice is the same whether you had Follicular Unit Extraction (FUE) or Direct Hair Implantation (DHI). While DHI may involve slightly smaller incisions and a different implantation tool, the graft fragility window is generally considered identical for both techniques.
In both cases, the transplanted follicles need the same 10–14 days to anchor securely. If you've had a combined procedure involving body hair grafts, your surgeon may provide additional donor-area guidance. However, the fundamentals — elevated back sleeping for 7–10 nights — apply to sleeping after FUE hair transplant and DHI procedures alike. Your surgeon may adjust specific recommendations based on graft placement and density.
Here's a quick comparison of sleep positions and their safety timeline:
Position |
Risk Level |
When It's Generally Safe |
Key Notes |
|---|---|---|---|
Back, elevated 30–45° |
Lowest risk |
Safe immediately; recommended from Night 1 |
Gold standard position for first 7–10 nights |
Back, slightly elevated ~30° |
Low risk |
After Night 7–10 |
Gradual step-down from full elevation |
Side sleeping |
Moderate risk |
After Day 10–14, with surgeon approval |
Risk depends on graft placement location |
Stomach sleeping |
Highest risk |
After Week 4 at the earliest |
Last position to reintroduce; consult your surgeon |

Night-by-Night Sleeping Timeline After Hair Transplant
Knowing the right position is one thing. Knowing when to adjust it — and what each night actually feels like — is another. This section walks you through exactly what to expect at each stage, so nothing catches you off guard. For a broader look at what's happening with your body each day, check out the day-by-day hair transplant recovery timeline.
Night 1: At the Clinic or Hotel in Istanbul
Your first night after the procedure is often the most restless — and that's completely normal. Adrenaline is still in your system, and mild discomfort from both the transplant area and the donor area keeps sleep light. Don't worry if you wake up several times.
You may still have bandaging on the donor area. Your clinic will typically provide a travel neck pillow to help keep your head stable. Sleep elevated on your back and resist the urge to touch or adjust the transplant area.
If your surgeon has prescribed pain medication or a mild sleep aid, take it before bed as directed. Many patients find that this first night is more about resting than truly sleeping — and that's perfectly fine.
Nights 2–3: Hotel Recovery in Istanbul
Bandages are usually removed after your first post-operative wash on Day 2. With the bandages off, you might feel more aware of the transplant area — but you'll also have more freedom of movement.
Swelling begins to build during this period, making elevation even more critical now. Request extra pillows from your hotel if needed, or continue using the travel pillow your clinic provided.
Place a clean towel over your pillow for these first few nights. Minor oozing or saline spray residue from the transplant area is normal and can stain your pillowcase. A fresh towel each night keeps everything clean and hygienic.
Nights 4–7: The Flight Home and First Week
Swelling typically peaks around Days 3–5. You may notice puffiness in your forehead or around your eyes — this is a normal part of the healing process and not a sign that anything has gone wrong. Staying elevated helps this swelling resolve faster.
If you're flying home during this window, see the flight home section below for specific tips on sleeping safely in transit. Once you're home, continue sleeping elevated at a 45-degree angle. If you have access to a recliner, this is the most comfortable option for many patients during this phase.
Here's the encouraging part: sleeping gets noticeably easier with each passing night. Discomfort decreases steadily, and by Night 6 or 7, most patients are sleeping reasonably well — even on their back.
Nights 8–14: Gradual Transition
By Day 10, your grafts are significantly more secure. The new blood supply is well established, and the risk of graft displacement from normal sleeping movements drops considerably.
During this phase, you can begin slightly reducing your elevation angle — from 45 degrees down to approximately 30 degrees. Your surgeon may also give you the green light to try gentle side sleeping, depending on where your grafts were placed.
Still avoid stomach sleeping during this period. And if you're unsure whether it's safe to change positions, contact your clinic. A quick message to their post-operative support team can give you peace of mind.
Week 3–4 and Beyond: Returning to Normal
Most patients can return to their normal sleeping position by Week 3–4. Side sleeping is generally comfortable and safe by this point. Stomach sleeping is the last position to reintroduce — typically after Week 4 at the earliest, though your surgeon may advise waiting longer.
The need to sleep elevated after hair transplant typically ends around this stage. Pay attention to how the transplant area feels when you change positions. If it still feels tender when you lie a certain way, continue sleeping elevated or on your back for a few more days. There's no downside to being cautious.
Here's a summary of the complete sleeping timeline:
Night / Week |
Recommended Position |
Elevation Angle |
Key Notes |
|---|---|---|---|
Night 1 |
Back only |
30–45° |
Bandaging may still be present; light sleep is normal |
Nights 2–3 |
Back only |
30–45° |
Swelling increasing; use towel on pillow |
Nights 4–7 |
Back only |
30–45° |
Swelling peaks Days 3–5; flight home during this window |
Nights 8–14 |
Back; gentle side sleeping possible |
~30° |
Grafts more secure; reduce elevation gradually |
Week 3–4+ |
Normal position gradually |
Flat or slight elevation |
Stomach sleeping last to reintroduce (Week 4+) |
Key takeaway: The first 7–10 nights are the most important. Sleep elevated on your back, then gradually transition as your grafts become secure and your surgeon gives the go-ahead.
Want a personalized recovery plan tailored to your specific procedure?
Talk to an experienced patient coordinator for your hair transplant in Turkey.8 Practical Tips for Better Sleep During Hair Transplant Recovery
You have your night-by-night plan. But even with the right position, falling asleep during recovery can be a genuine challenge — especially if you've spent your entire life sleeping on your side or stomach. These eight tips will help you sleep more comfortably and protect your grafts at the same time.
1. Invest in a Wedge Pillow or Use a Recliner
A wedge pillow for hair transplant recovery maintains a consistent elevation angle throughout the night, unlike stacked pillows that can shift or flatten as you sleep. If you don't have a wedge pillow, a recliner set to roughly 45 degrees is often the most comfortable option during the first week. Set up your sleep environment before your procedure day so everything is ready when you get home.
2. Use a Travel Neck Pillow to Prevent Head Rolling
A U-shaped neck pillow keeps your head centered and prevents unconscious rolling to one side during the night. This is especially helpful during the first 5–7 nights, when staying on your back is most critical. Your clinic may provide one — if not, pick one up before your procedure.
3. Place Pillows Along Your Sides as Barriers
Imagine it's 3 a.m. and you're deeply asleep. Your body naturally tries to roll into its usual position. Placing body pillows or firmly rolled towels along both sides of your torso creates a physical barrier that reminds your body to stay put — even while you're unconscious. This simple setup is one of the most effective graft-protection strategies you can use.
4. Protect Your Pillowcase
Use a clean, soft pillowcase — silk or satin is ideal because it creates less friction against the transplant area than cotton. Friction can irritate healing skin and potentially disturb grafts in the earliest days. For the first 3–5 nights, lay a clean towel over the pillowcase as an extra layer of protection against minor oozing or residue.
5. Take Prescribed Medications on Schedule
If your surgeon has prescribed pain medication or anti-swelling medication, take it at the recommended time — ideally 30 minutes before bed. Staying ahead of discomfort is far easier than trying to catch up once pain has set in. Some surgeons prescribe a mild sleep aid for the first 2–3 nights. Take it only as directed, and never take any sleep medication your surgeon hasn't approved.
6. Keep the Room Cool
Overheating increases scalp sweating, which can irritate the transplant area and make sleep more difficult. Keep your bedroom temperature between 18–20°C (64–68°F). A cool room also promotes deeper, more restful sleep — something your body needs during recovery.
7. Avoid Alcohol and Caffeine Before Bed
Alcohol thins the blood and can increase swelling. Caffeine disrupts sleep quality during a period when falling asleep is already harder than usual. Avoid both for at least 7–10 days after your procedure. Water and herbal tea are better choices in the evenings.
8. Set a Gentle Alarm if You're a Restless Sleeper
If you tend to toss and turn, consider setting a soft alarm every 3–4 hours for the first 2–3 nights. This lets you check your position and readjust if needed. It's not mandatory — pillow barriers are typically sufficient on their own. But for very restless sleepers, it provides a valuable extra layer of protection.
What if you simply can't fall asleep on your back? You're not alone. This is one of the most common frustrations patients report. If you've spent a lifetime sleeping on your side or stomach, the adjustment can feel impossible at first. Try combining the recliner option with a neck pillow for the first few nights — the reclined angle often feels more natural than lying flat on stacked pillows. If sleep remains difficult after 2–3 nights, contact your surgeon. They may be able to recommend a mild, approved sleep aid to help you through the hardest stretch.
Bottom line: Preparation is everything. Set up your sleep environment before your procedure, and you'll remove the guesswork from your recovery nights.

What Happens If You Accidentally Sleep on Your Grafts?
This is the question that keeps more patients awake than any physical discomfort. You've set up your barriers, followed every tip — and then you wake up at 3 a.m. on your side, heart pounding. The fear is understandable. Let's address it directly.
How Resilient Are Your Grafts, Really?
Here's the reassuring reality: a single brief moment of rolling onto your side is unlikely to destroy your results. Grafts are more resilient than most patients expect. The real risk comes from repeated or prolonged pressure on the transplant area — not a momentary shift during the night.
A brief position change — the kind where you wake up and immediately realize you've moved — is very different from spending hours face-down on your transplant area. Your body's healing response begins immediately after the procedure, and even in the first few days, grafts have some degree of initial stability in their recipient sites.
Steps to Take If You Wake Up in the Wrong Position
If you wake up and realize you've shifted, here's what to do:
Gently reposition yourself onto your back. Do not panic.
Do not touch, press, or rub the transplant area.
Check your pillow for any unusual bleeding — a small amount of spotting in the first few days is normal, but significant fresh blood is not.
Look for visibly displaced grafts, though this is rare from a brief position change.
Contact your clinic if you notice anything concerning — visible graft displacement, persistent bleeding, or significant pain.
Reputable clinics provide post-operative support for exactly these situations. Don't hesitate to reach out, even if it's the middle of the night.
After Day 10, the risk from accidental position changes is very low. This is precisely why the pillow barrier method and neck pillow are so valuable — they prevent the situation from happening in the first place, so you can sleep without that gnawing anxiety.
Sleeping Tips for the Flight Home After Hair Transplant in Turkey
The flight home presents its own challenge. Whether it's a 3-hour hop to Europe or a longer intercontinental journey, your sleep position on the plane still matters — and you have less control over your environment than you do in a bed.
Here are specific tips for sleeping safely during your flight:
Bring a travel neck pillow. Your clinic may provide one. Wear it throughout the flight to keep your head upright and stable.
Choose an aisle seat if possible. This gives you more room to keep your head centered and avoids the temptation to lean against the window — pressing your transplant area against a hard surface.
Don't recline your seat fully. A slight recline is fine, but avoid going nearly flat. Keep your head elevated above your heart.
Wear the headband your clinic provides. This forehead band helps direct swelling downward and away from the eye area — especially useful during flights when you can't control your elevation angle as precisely.
Stay hydrated. Cabin air is dry, and dehydration worsens swelling. Drink water regularly throughout the flight and avoid alcohol entirely.
Adjust your position periodically. On flights longer than 4 hours, shift your weight and gently move your neck every hour or so to prevent stiffness and maintain circulation.
If the passenger next to you falls asleep and leans toward you, gently adjust your position to protect the transplant area. Most fellow travelers will understand if you briefly explain that you've had a medical procedure.
Frequently Asked Questions About Sleeping After Hair Transplant
The general recommendation is a minimum of 7–10 nights of sleeping elevated at a 30–45 degree angle. Some surgeons advise maintaining slight elevation for up to 14 nights. After that, you can gradually reduce the angle. Your surgeon may adjust this timeline based on your specific graft placement and healing progress.
Yes. Stack 2–3 firm pillows to create a stable incline. The key is maintaining a consistent angle throughout the night. Wedge pillows are preferred because they don't flatten or shift, but stacked pillows work well if you arrange them securely and check them before falling asleep.
Most patients return to their normal sleeping position by Week 3–4. Side sleeping is typically safe after Day 10–14 with surgeon approval. Stomach sleeping should wait until at least Week 4. If any position still causes discomfort, continue sleeping elevated until it feels comfortable.
Sleeping without any elevation is not recommended until at least Week 3–4. Even then, most surgeons suggest using at least one pillow for comfort as the transplant area continues to heal. If you prefer sleeping completely flat, confirm with your surgeon that your grafts are fully secure before making the switch.
Yes — napping is fine and even encouraged. Your body heals faster with rest. The same elevation rules apply during naps: sleep elevated on your back, even for a short rest. Don't nap face-down on a couch or flat on a bed without proper pillow support.
Exercise caution during the first 7–10 days. A partner or pet can accidentally bump, press, or roll against your transplant area during the night. Many patients choose to sleep alone for the first week. If that's not practical, use pillow barriers to create a protective buffer around your head and communicate the importance of careful movement to your partner.
Consult your surgeon before your procedure about CPAP use during recovery. The mask straps may need adjustment to avoid pressing on the transplant area or donor area. Your surgeon can advise whether modifications are needed or whether an alternative sleeping arrangement is preferable for the first few nights.
When to Contact Your Clinic About Sleep-Related Concerns
Most sleep-related discomfort resolves on its own within the first week. But some symptoms go beyond normal recovery and require prompt attention. Contact your clinic if you experience any of the following:
● Excessive or worsening swelling after Day 5 that does not improve with continued elevation
● Visible graft displacement — grafts that appear to have shifted or fallen out after sleeping
● Persistent or significant bleeding on your pillow beyond the first 2–3 nights
● Severe pain that disrupts sleep beyond the first 3–4 nights and doesn't respond to prescribed medication
● Signs of infection at the transplant or donor site, including increasing redness, warmth, unusual discharge, or fever
Reputable clinics — especially those experienced with international patients — provide 24/7 post-operative support by phone or messaging. No question is too small when it comes to protecting your results. If something feels wrong, reach out.
Your Sleep Will Return to Normal — and So Will Your Confidence
The first week of sleeping after a hair transplant is genuinely uncomfortable. There's no point pretending otherwise. But here's what matters: these restrictions are temporary. The results are not.
Keeping your head elevated at 30–45 degrees for those first 7–10 nights is the single most impactful thing you can do to protect your grafts and support your healing. Every night of careful positioning brings you closer to the point where none of this is necessary anymore.
Within a few weeks, you'll be sleeping however you like. Within a few months, you'll start seeing new growth that makes these temporary adjustments more than worth it. The discomfort fades. The results stay.
If you're still in the planning stages, a free consultation can help you understand exactly what your recovery — including sleep — will look like for your specific case. Getting answers now means fewer surprises later.


