Hair Transplant Infection: Warning Signs, Prevention & Treatment
Tip: Replace “Licensed Physician Reviewer” with the surgeon/doctor name + credentials (e.g., “MD, Hair Transplant Surgeon”) for stronger medical EEAT.
Often cited rate of true infections with modern sterile technique
Typical onset window after a procedure
Common timeframe to see improvement after correct treatment
Typical recovery when managed early
ℹ️ Medical Disclaimer
This article is for educational purposes and does not replace medical advice. If you suspect an infection after hair transplant surgery, contact your clinic or a qualified healthcare professional promptly—especially if you have fever, increasing pain, spreading redness, or pus.
MedArt Hair Clinic: What We See Most Often in Real Aftercare
In our clinical follow-ups, infections are uncommon when patients follow the first-week washing and hygiene protocol. When problems do occur, the most frequent triggers are touching or scratching grafts, delaying the first guided wash, using non-approved topical products, and sleeping with unclean bedding or hats during the early healing phase.
If you want maximum trust (and better Google rankings), add your verified clinic statistic here: [Insert your verified infection rate / audited clinic data] and keep it consistent across the website.
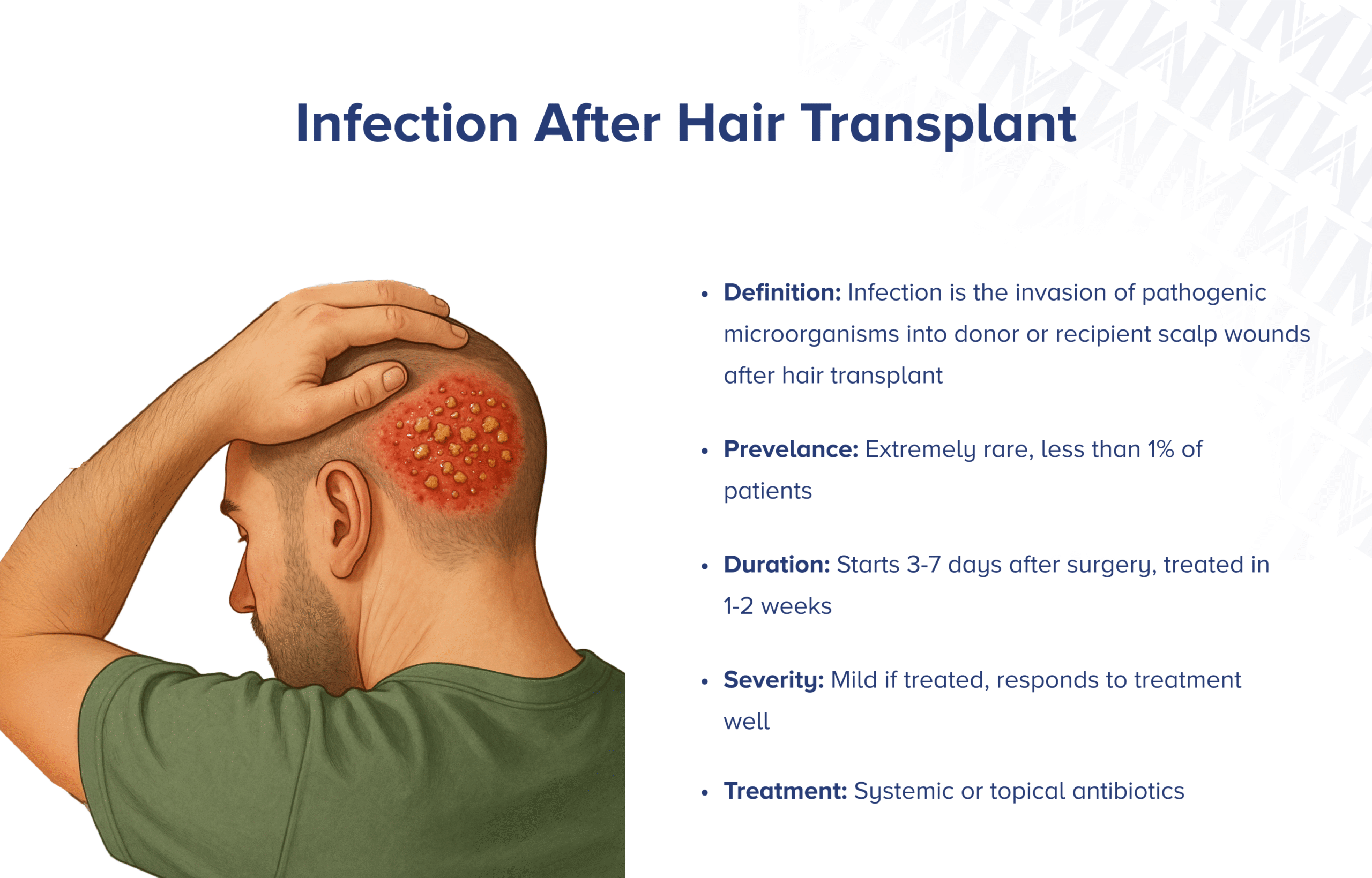
Hair transplant infection is a rare but important complication where bacteria invade donor or recipient scalp wounds, causing inflammation, pus formation, and potentially affecting healing. While most patients heal normally, recognizing infection early and acting quickly is the best way to protect your results.
This guide covers how to recognize warning signs, the most common causes, proven prevention steps, and what treatment typically looks like. If you want to strengthen your aftercare overall, also read our guides on hair washing after hair transplant and post-op medication.
Key Points
- True infections after hair transplant are generally uncommon with sterile technique and correct aftercare.
- Symptoms often appear 3–7 days after surgery and include increasing pain, warmth, spreading redness, and pus.
- Most cases improve quickly with early medical evaluation and appropriate treatment.
- Risk factors include diabetes (poor control), smoking, poor hygiene, excessive crusting, and immunosuppression.
- Prevention is mainly about first-week hygiene, clean bedding, approved products only, and not touching grafts.
- When needed, treatment may include culture-guided antibiotics and (rarely) drainage of an abscess.
- Prompt action matters to reduce risk of graft loss, scarring, or wider spread infection.
✅ Worried about infection risk?
If you have redness, warmth, pus, or increasing pain, don’t wait. Contact your clinic and send clear photos for medical evaluation.
MedArt tip: Take photos in good lighting from the same angle each time so your team can track changes accurately.
What is a hair transplant infection?
A hair transplant infection occurs when bacteria enter healing donor or recipient sites and cause inflammatory tissue damage beyond normal post-operative healing. Normal healing tends to improve day-by-day; infection tends to worsen after the initial 2–3 days and may include pus, spreading redness, warmth, and increased pain.
During a hair transplant, hundreds to thousands of small sites are created. These sites heal safely when sterile technique and correct aftercare are followed. Infection risk rises when bacteria have a chance to multiply—most commonly from contamination (hands, hats, pillowcases), delayed or improper washing, or using non-approved products.
What are the signs and symptoms of hair transplant infection?
Early recognition is the key. Here is what to watch for:
Early warning signs:
- Increasing pain that gets worse instead of better after the first few days
- Spreading redness beyond the immediate donor/recipient zone
- Warmth to touch (noticeably hotter than surrounding skin)
- Swelling that increases rather than decreases
Progressive symptoms:
- Thick yellow/green drainage (pus)
- Foul-smelling discharge
- Red streaking extending away from the area
- Increasing tenderness that disrupts sleep
Urgent signs:
- Large painful bump (possible abscess)
- Fever, chills, or feeling generally unwell
- Rapid spread of redness/swelling across the scalp
⚠️ Quick Self-Check
Normal healing: symptoms are stable or improving each day.
Possible infection: symptoms worsen after day 2–3, especially with pus, spreading redness, warmth, or fever.
How common is infection after hair transplant?
📊 Generally Uncommon With Modern Standards
With sterile technique and correct aftercare, infection after hair transplant is generally uncommon. Your personal risk depends on health factors (e.g., diabetes control), smoking, and how strictly you follow aftercare instructions.
Why infections are usually uncommon:
- Clinic sterile protocols and single-use/disinfected instruments
- Minimally invasive techniques (especially modern FUE)
- Guided washing and aftercare reduces contamination risk
- Early follow-up helps identify issues before they escalate
If you are researching procedures, you may also find it helpful to compare techniques. See: FUE Hair Transplant in Turkey and DHI Hair Transplant in Turkey.
How long does an infection last after a hair transplant?
Duration depends on how quickly you start appropriate treatment. When an infection is recognized early, you often see improvement within 24–48 hours after the correct treatment plan is started, with resolution commonly within 1–2 weeks.
Typical timeline:
Onset: often within 3–7 days after surgery
Response: improvement may begin within 24–48 hours after appropriate management
Resolution: commonly within 1–2 weeks (varies by severity)
What causes infection after hair transplant?
Most causes are practical and preventable. In real aftercare, contamination usually happens through hands, textiles, or unapproved products.
Post-Operative Hygiene Issues
Touching the scalp with unwashed hands, delaying the first guided wash, using non-approved shampoos/lotions, or reusing towels can increase contamination risk.
Wound Care Problems
Excessive crusting may trap debris and bacteria. Aggressive rubbing can disrupt healing sites. Picking scabs is a frequent trigger for irritation and secondary infection.
Patient Risk Factors
Diabetes (especially if poorly controlled), smoking, immune suppression, and certain skin conditions can increase risk and slow healing.
Environmental Contamination
Unclean pillowcases, hats/helmets, swimming pools/hot tubs too early, and close contact with pets directly against healing sites can raise risk.
Who is more likely to develop an infection after a hair transplant?
Some patients have higher baseline risk, so prevention and follow-up are even more important.
- Medical Conditions - Diabetes (poor control), immune compromise, chronic skin inflammation
- Medications - Immunosuppressants (e.g., steroids), certain therapies that reduce immune response
- Lifestyle Factors - Smoking, heavy alcohol use, poor nutrition, low sleep quality
- Aftercare Behavior - Picking scabs, scratching, using unapproved products, unclean bedding/hats
How is a hair transplant infection diagnosed?
Clinicians diagnose infection through visual examination and symptom pattern. When discharge is present or symptoms are significant, a bacterial culture may be used to guide antibiotic choice.
Physical Examination
Signs include progressive spreading redness, warmth, swelling, tenderness, and purulent discharge.
When cultures are helpful
If the infection is moderate/severe, recurrent, or not improving as expected, a clinician may sample discharge for culture and sensitivity testing.
How serious is a hair transplant infection?
Most cases are manageable if treated early. Serious outcomes are more likely when symptoms are ignored, treatment is delayed, or the patient has high-risk conditions.
⚠️ Severity Overview
• Mild cases: limited area, respond well to early treatment, usually no effect on final results.
• More serious cases (rare): abscess formation requiring drainage, increased risk of scarring, and potential graft loss if untreated.
• Emergency: fever + rapidly spreading redness, severe illness, confusion, or breathing difficulty—seek urgent care.
How to prevent hair transplant infections?
✅ Prevention Checklist (Practical + Clinic-Based)
Prevention is mostly about your first-week routine. The goal is to keep healing sites clean without trauma.
- Follow the first wash instructions: Use clinic-approved shampoo and gentle technique. See our guide: Hair Washing After Hair Transplant.
- Keep hands off: No scratching, no picking scabs, no rubbing.
- Clean environment: Fresh pillowcases daily, clean towels only, avoid hats/helmets unless your clinic approves.
- Avoid water risks: No pools, oceans, hot tubs until your clinic clears you (commonly ~2 weeks).
- Health factors: Stop smoking if possible, keep blood sugar controlled, sleep well, stay hydrated.
- Approved products only: Avoid random oils/creams/sprays unless prescribed by your clinician.
How to treat a hair transplant infection?
Immediate Steps
- Contact your clinic promptly: Early evaluation protects results.
- Document symptoms: Clear photos in good lighting help clinicians assess severity.
- Avoid self-treatment: Don’t use leftover antibiotics or harsh topical products.
- Continue gentle hygiene: Follow clinic instructions until you are evaluated.
Medical Treatment
Treatment depends on severity and may include oral antibiotics, topical care, and (when needed) culture testing to select the most effective antibiotic. In rare cases with an abscess, drainage may be required by a qualified clinician.
What to Expect
Many patients notice early improvement within 24–48 hours after appropriate management begins. If symptoms do not improve as expected, a re-check is important.
Will a hair transplant infection go away completely?
In most cases, yes—when treated early and correctly, infections resolve completely. The goal is to manage the infection quickly before it disrupts healing or affects grafts.
Impact on Results
- Most treated infections do not change final results
- Hair growth may be delayed in the affected area
- Severe/untreated infection increases risk of scarring and graft loss
When to see a doctor for hair transplant infections?
⚠️ When to Seek Medical Attention
Contact your clinic promptly if you experience:
- Increasing pain after day 2–3
- Spreading redness beyond the surgical sites
- Pus (yellow/green discharge) or foul odor
- Fever or feeling unwell
- Rapid worsening of any symptoms
Seek urgent care if you have:
- High fever with chills or severe illness
- Rapidly spreading infection across large areas
- Confusion, very fast heart rate, or difficulty breathing
Early evaluation almost always leads to better outcomes and protects your hair transplant investment.
Real-World Examples (Optional but Highly Recommended)
🖼️ Add Verified Clinic Images for Trust
For stronger trust and better rankings, add real clinical images (with patient consent) or educational diagrams:
- Example: mild localized infection (Day 5) successfully treated
- Example: normal healing vs infection comparison
- Example: correct washing technique photos
Implementation tip: Use descriptive alt text like “Hair transplant infection early signs on recipient area” and add a short caption.
References (Evidence & Medical Trust)
For best medical EEAT, include references from recognized sources. Add your preferred citations here (PubMed/clinical journals/ISHRS). Examples you can replace with your exact sources:
- International Society of Hair Restoration Surgery (ISHRS) – patient safety and aftercare guidance (replace with exact page/title).
- Peer-reviewed dermatologic surgery literature on postoperative infection prevention (replace with DOI/PMID).
- Clinic protocol documents (internal): sterile technique + aftercare checklist (if publicly shareable).
Important: Do not claim a specific “<1%” rate as a clinic statistic unless you can verify it with audited internal data or a credible published source.